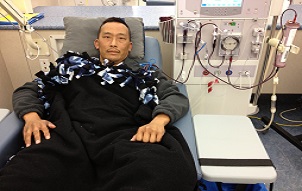
Living donation involves anesthesia and major surgery and their associated risks.
In the majority of cases, the surgical removal of the donor’s kidney (called a donor nephrectomy) is done by laparoscopic surgery which involves two to three small incisions in the abdomen and one larger incision (6-9 centimeters) through which the kidney is removed. Surgery is performed under general anesthesia. In a small number of cases, a laparoscopic nephrectomy is not an option, so the surgery involves a five to seven inch incision on the side of the chest and upper abdomen.
Surgical complications can include pain, infection, blood loss (requiring transfusions), blood clots, allergic reactions to anesthesia, pneumonia, injury to surrounding tissue or other organs, and even death.
After surgery, the remaining kidney will grow slightly larger to make up for some of the function of both kidneys. Some people are born with one kidney or lose one due to injury and are able to live full lives with little or no effect. However, people with one kidney may be at a greater risk of high blood pressure, proteinuria (protein in the urine) and reduced kidney function. In very rare cases, a kidney donor may experience loss of kidney function in the years following their kidney donation. Should this occur, priority is given to a prior living donor according to national organ transplant waiting list regulations.
Please note that there has been no national systematic long-term data collection on the risks associated with living organ donation. Based upon limited information that is currently available, overall risks are considered to be low – 95 to 96 percent of donors have no complications.
A study by Johns Hopkins University School of Medicine that followed 80,000 living kidney donors over a 15-year period found that there was no increase in mortality rates among donors compared to healthy people with both kidneys.
In a 2015 paper published in the Journal of the American Society of Nephrology, lifetime risk for the average person of ESRD was 326/10,000 (about 1 in 30), 90/10,000 (about 1 in 110) for those who donated a kidney, and 14/10,000 (about 1 in 700) for healthy non-donors. The reason kidney donors have a lower risk of ESRD compared to the general population is that kidney donors are typically healthier than the average person due to the donor screening process. When donors and healthy non-donors are compared, there is an implied ESRD risk increase of 76/10,000 from donating a kidney. The following are informative papers related to long term risks of donating a kidney: (Source: National Kidney Registry)
Journal of the American Society of Nephrology – 2015
Reassessing Medical Risk in Living Kidney Donors
Journal of the American Medical Association – 2014
Risk of End-Stage Renal Disease Following Live Kidney Donation
New England Journal of Medicine – 2009
Long-Term Consequences of Kidney Donation
Some medical organizations, such as the American Academy of Sports Medicine and the American Academy of Family Physicians, suggest that a person with one kidney should refrain from sports involving high contact or frequent collisions. Individuals who participate in these sports should exercise caution, be aware of possible consequences, and wear appropriate protective equipment.
Negative psychological symptoms are also possible during the healing process and even years after the donation. Your donated organ may not function in the recipient after it is transplanted. You and/or the transplant recipient may have medical problems from the surgery. Scarring or other aspects of the donation process could possibly contribute to problems with body image. You may have feelings of regret, resentment, or anger. You may have symptoms of anxiety or depression. Treatment for these conditions can be lengthy, costly, and could possibly include the use of medications with risks and side effects.
Some donors have reported difficulty in getting, affording, or keeping health, disability, or life insurance. It is important that you talk with your own insurance carriers before making a decision about being a living donor. Your premiums could increase. If you do not have health insurance, serving as a donor could be considered a pre-existing condition if you apply for insurance later.
If you work, talk with your employer about any existing leave policies before committing to living donation. Also, fully think about the financial impact on your family, especially if you and/or whoever serves as your caregiver during the donation recovery process may face lost wages.
Source: UNOS Living Donation